A traditional path to a drug addiction problem might sound like this: First, the person makes a choice to use a drug just one time, just for fun. Next, the person finds that feelings of sickness appear when drugs aren’t taken. And finally, the person feels both a physical and a psychological need for drugs that takes over almost every aspect of the person’s life. That is a typical progression, but as Robin L. Hoover, RN, MSN, CADCi, Director of Nursing at American Addiction Centers, points out, addiction can be variable
“The condition of addiction knows no boundaries in terms of age, gender, socioeconomic status, education, profession,
religion, culture, marital status, etc…An addicted person’s motivation to seek treatment and embrace recovery is as broad
and varied as the population of sufferers themselves.”
But one thing that might motivate people to get care, or to stick with treatment plans once they start, involves the health complications addiction can deliver.
“Health complications are among the motivational factors, but certainly not necessarily the most convincing and rarely the sole rationale,” Hoover cautions. “Many other factors come in to play for most addicted people, such as legal, financial, relationship, child custody, job/professional, family pressure, loss of loved ones through drug use, loss of basic needs (e.g., food, shelter, clothing), and more. But in my experience, the more mature addicts perceive health complications as a worthy inspiration.”

That means it might behoove families to understand the health complications associated with addiction, so they can provide loved ones with addictions a reason to consider entering rehab. Should that addicted person agree to treatment, that information could help people to stick with care once it starts.
Complications by Length of Use
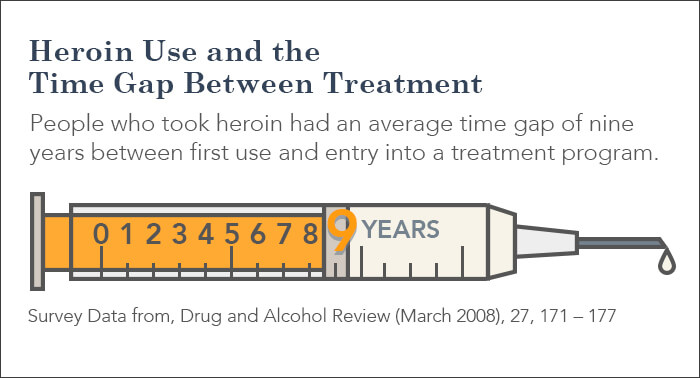
Some people march right into treatment plans early in the addiction process. But it’s not at all unusual for people to live with addictions for very long periods of time before they get the help they need. For example, in a study in the journal Drug and Alcohol Review, researchers found that people who used heroin had an average time gap of nine years between first use and entry into a treatment program. What this indicates is that some people may spend about a decade using drugs before they get help, and they can face very specific health complications every step of the way.
Immediate & Short-Term Health Concerns
People may face various acute health risks immediately after drinking or using a drug. When asked about such immediate risks of drug use, Hoover came up with 28 different types of consequences, ranging from mild (e.g., drowsiness, confusion) to severe (e.g., loss of consciousness, tremors). She points out that some immediate consequences can lead to other types of consequences in time.
“The immediate complications may create new health risks, such as increased risk for falls, accidents, sharing needles (leading to abscesses, hepatitis C, or HIV), and sexual promiscuity (leading to HIV, STDs, and unwanted and high-risk pregnancies)”.
The most serious immediate concern involves overdose, and according to the National Institute on Drug Abuse, more than 17,000 people died in 2017 due to an overdose of prescription opioids. Many more lost their lives to overdoses on other widely abused substances including heroin, fentanyl, cocaine, psychostimulants or other prescription drugs (e.g., benzodiazepines and antidepressants). Sometimes, the drugs suppress breathing, so people slide into deep sleeplike states.
Overdoses occur when the toxic effects of a drug overwhelm the individual using the substance. Sometimes the drugs suppress breathing or stop breathing altogether. Sometimes the drugs dangerously increase blood pressure and heart rate, which can tax the cardiovascular system to such a degree that heart attack or stroke may occur. And sometimes, the drugs elicit such profound sedation that a person loses consciousness.
In addition to the physical health concerns associated with the immediate use of drugs, people who use these substances can also experience very strange, altered states of perception, as well as disturbing auditory or visual hallucinations (i.e., seeing things others can’t see or hearing voices others cannot hear).
While under the influence of drugs, these people might run into traffic, attempt to drive or operate heavy machinery, or take on some other task that can lead to an accident. Sometimes, people under the influence commit criminal or violent acts, and then face law enforcement action. These immediate consequences may not be explicitly linked to health, but it’s easy to see how they might have an impact on a person’s overall physical condition.
In addition, some drugs lead to a significant physiological dependence and, when attempts are made to quit or cut back on use, severe withdrawal symptoms can make it difficult to maintain abstinence. People who feel anxious, agitated, or physically ill after stopping a drug may use again just to make the discomfort stop, and that can set them up for a lifetime of using and abusing drugs.
Longer-Term Health Concerns
In-depth Reading
Immediate health consequences are easy to understand, and they can be very hard to ignore. But some health impacts tied to drugs aren’t as clear-cut. Specifically, some health issues are tied to continued use of the drug over a period of several weeks or months.
These longer-term health concerns can be quite serious. Consequences associated with longer-term use of drugs include a higher risk of chronic conditions and increased cumulative risk of acute issues as long as substance use continues. A 2017 study published in the Journal of Addiction Medicine, found 19 common health conditions were higher in patients with substance use disorders vs. demographically matched patients without a history of drug or alcohol abuse, including arthritis, asthma, chronic pain, congestive heart failure, hypertension, pneumonia, and stroke. These patients also had an elevated risk of dying—and at a younger age—than those without a substance use disorder.
Other longer-term health concerns for those who abuse drugs revolve around drug-seeking behavior; that is, when people spend a great deal of time getting, taking, and sharing drugs. This results in neglecting personal care and hygiene. For example, people using drugs at this level may not eat nutritious meals on a regular schedule, or they may just eat fast-food. They may lose a great deal of weight, and they may start to experience dental health issues, too.
In addition to a higher risk of chronic and acute disease, other longer-term health consequences associated with continued drug use includes contraction and spreading of STDs and other infectious diseases. For example, HIV or hepatitis can spread when people who inject drugs share needles with one another. The tiniest drop of blood left inside a needle has the power to infect another person. In fact, the Centers for Disease Control and Prevention reports that people who inject drugs accounted for 9% of diagnoses of HIV in the United States in 2016.
It’s important to note, too, that the risk of disease transmission isn’t only associated with injected drugs like heroin. AIDS.gov reports that alcohol, methamphetamine, crack cocaine, and club drugs like MDMA (“ecstasy” or “Molly”) have all been linked to a boost in STD transmission.
Some people develop HIV and hepatitis as an STD through unsafe sex practices. While under the influence of drugs or alcohol, users can have lower inhibitions, making it easy for them to make poor decisions about their health, such as abandoning the use of condoms or other safe sex practices.
STDs and infectious diseases can certainly be part of longer-term health consequences associated with drugs, and although many can be successfully treated with medications, addiction can make life so chaotic that sticking to a medication routine can be very difficult for people to accomplish. Some people who have these types of diseases blame their symptoms on the drugs they continue to take
Although negative health consequences are associated with routine drug use, no matter the substance, there are some health issues that are exclusively tied to one particular type of drug.
Sedatives/Depressants
In-depth Reading
Alcohol, barbiturates and benzodiazepines such as diazepam (Valium) and alprazolam (Xanax), are considered central nervous system depressants. These drugs slow neural processes in the brain, and while under the influence, people may seem sedated, sleepy and slow. They may also:
- Slur speech;
- Stagger while walking;
- Breathe slowly;
- Have lowered blood pressure; and
- Experience headaches, light-headedness, or dizziness.
If taken in large enough doses, or in combination with one another, depressants can lead to coma and death. In lower doses, people can be cut off from their emotions and feelings. They may feel emotionally blunted, and that could lead to relationship distress. A loss of personal connections could lead to a boost in drug use, and that could lead to overdose.
CNS depressants are also associated with significant physiological dependence, and when people attempt to stop their use, they can experience potentially life-threatening complications, according to the National Institute on Drug Abuse. A brain long sedated by depressants can be unprepared for their sudden removal, requiring a slow and steady detox approach. Withdrawal symptoms, sometimes severe and potentially life-threatening, can develop as early as a few hours after the drug was last taken. These include:
- Seizures;
- Shakiness;
- Anxiety;
- Hallucinations; and
- Increased heart rate, blood pressure, and temperature with sweating.
Dissociatives/Hallucinogens
Drugs like PCP, ketamine, dextromethorphan (DXM or DM), LSD (“acid”), DMT, peyote and so-called magic mushrooms tinker with brain chemistry, resulting in pronounced sensory and perceptual disturbances and, in some cases, dissociation—an impaired self-awareness resulting in feelings of detachment from the self and a distortion in what people see, feel, and experience.
“Hallucinogenic drugs by definition distort the perception of reality, which in itself can be very dangerous,” Hoover says. “And these drugs are unpredictable, making them all the more dangerous.”
The mind-altering effects of these substances may seem pleasant to the person choosing to take drugs, especially if the drug use takes place in a safe space, but they definitely pose short-term health risks.
“Some people don’t believe they are as addictive as other drugs, and there may be some truth to that,” Hoover says. “However, they can cause significant changes in blood pressure, heart rate, and body temperature. People who take them can experience sleeplessness, weight loss, decreased appetite, depression, profuse sweating, decreased muscle coordination, and numbness in the extremities.”
In addition to these short-term effects, the National Institute on Drug Abuse reports that some of these drugs can result in longer-term alterations in perception or hallucinations. People who experience Hallucinogen Persisting Perception Disorder (HPPD), often referred to as flashbacks, can experience visual disturbances (seeing “halos” or “trails” attached to moving objects) or be thrust into the middle of a hallucination at completely inopportune times, including when they’re working or driving, and they may become so afraid of the next episode that they develop symptoms of an anxiety disorder.
Opioids
In-depth Reading
Opioids like hydrocodone (Vicodin, Norco), oxycodone (OxyContin), morphine, codeine and others are commonly prescribed to relieve acute pain, but they also activate reward regions in the brain making them highly addictive and giving them a high potential for misuse and abuse. Some people who were legally prescribed an opioid for a legitimate health concern begin to compulsively misuse these medications and may turn to illegally obtained opioids, such as heroin, when they are no longer able to obtain the pharmaceutical product.
Many of the health concerns associated with opioids are immediate, as this class of drugs is closely associated with overdose and death. The Centers for Disease Control and Preventionreports that opioids were involved in 47,600 deaths in 2017, and opioid overdose deaths were six times higher in 2017 than in 1999. But an overdose isn’t the only risk associated with opioid abuse.
People who take opioids may experience episodes of slow, shallow, or stopped breathing, because the drugs interact with parts of the brain stem that control breathing. The National Institute on Drug Abuse suggests that long-term use of opioids can cause short-term respiratory depression and long-term damage to brain functioning. In time, people may have lasting damage that could impair decision-making abilities.
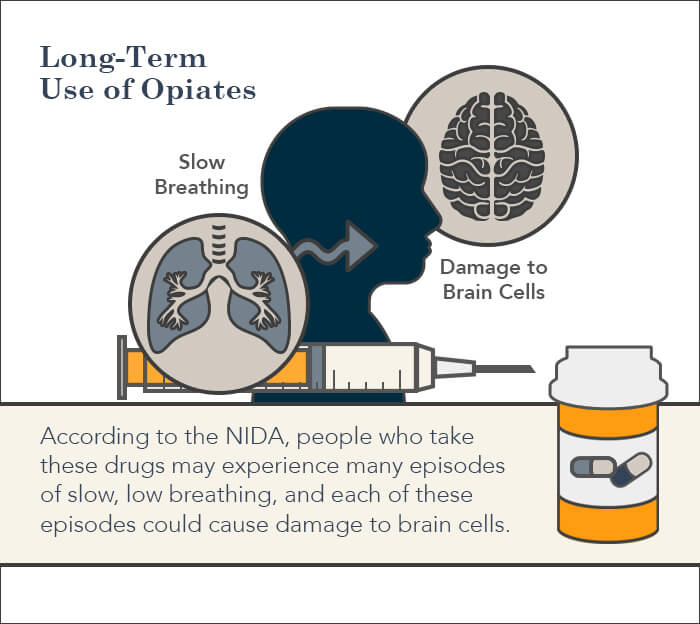
Opioids can also impact cells in the digestive tract, slowing the movement of food and water leading to constipation. After years of constipation, some people may develop additional gastrointestinal issues such as bowel obstruction and tears.
Stimulants
In-depth Reading
Illicitly abused cocaine and methamphetamine, as well as prescription stimulants used to treat attention-deficit hyperactivity disorder (ADHD) or narcolepsy (e.g., Ritalin, Adderall, Dexedrine) increase alertness, attention and energy. People using these substances may also experience:
- Increased blood pressure and heart rate;
- Increased breathing; and
- Vasoconstriction and decreased blood flow.
Users of these substances put their hearts through repeated episodes of strain and stress as their addictions grind on. High doses and long-term use can lead to dangerously high body temperature, exhaustion, reduced sexual functioning, cardiovascular damage, an irregular heartbeat, and seizures. Longstanding abuse may also lead to tissue death inside the heart and cardiovascular system, and that make heart attack, cerebral hemorrhage, or stroke more likely.
In addition, according to the Substance Abuse and Mental Health Services Administration, long-term use of stimulants can lead to persistent anxiety, hallucinations, delusions, paranoia and depression.
What drugs cause the most health complications?
Every drug comes with its own set of risks and complications. Researchers often like to compare one drug to another, in terms of its dangers. In one such research article published in The Lancet and highlighted by The Economist, researchers determined that heroin was the most harmful drug to the users themselves, while alcohol was the most harmful drug for others. It’s best to remember, however, that every drug can be dangerous, depending on the person taking that drug. And even so-called “safer” or prescription drugs can be deadly if taken in high doses or in combination with other drugs.
What is acetaminophen toxicity?
Acetaminophen is an over-the-counter medication that can alleviate mild-to-moderate pain and reduce fever. Many prescription painkillers are formulated with a combination of acetaminophen with opioids (e.g., Percocet, Vicodin, Norco). People who become addicted to these combined medications may begin to compulsively misuse them due to the reinforcing effect of the opioid, but they may take in a great deal of acetaminophen each day, as the two drugs are combined in the same pill.
According to the Food and Drug Administration (FDA), adults taking more than 4 grams of acetaminophen in a day can cause serious liver damage due to acetaminophen toxicity. That damage can be so severe, in fact, that it can cause death. In 2013, the FDA also warned the public that acetaminophen has been associated with a risk of rare but serious skin reactions. Additionally, the threshold for acetaminophen-related liver injury is considerably lowered when alcohol is concurrently used.
What’s worse on the body: smoking or injecting drugs?
Make no mistake: All methods of drug use can be intensely hard on the health of the body, and there are negative and potentially life-threatening health consequences regardless of whether a drug is smoked, snorted or injected.
“An injection crosses the blood/brain barrier directly and rapidly, increasing addictive qualities,” Hoover says. In a study of 400 people who abused methamphetamine on a regular basis, published in the journal Drug and Alcohol Review, researchers found that people who injected the drug had higher levels of drug dependence than those who smoked the drug. That’s likely due to the speed with which injecting puts a drug in contact with the cells of the brain. That speed causes a huge reaction inside the brain, and that big shift could lead to a quick development of addictive tendencies.
Injecting drugs can lead to serious health problems. A study published in the British Journal of Dermatology reported that 11% of IV drug users had at least one skin abscess within a 6-month period.
In addition to skin infections, some people who inject drugs develop scarring in veins and arteries due to long-term needle use. Injected foreign particulate matter can increase the likelihood of chronic vascular inflammation, heart attacks or strokes, People who inject drugs and share needles run the risk of endocarditis, an infection of the inner lining of the heart, or contracting blood borne diseases like hepatitis and HIV.
Some people choose to smoke their drugs, igniting them and breathing in the vapors. Drugs like crack cocaine are terribly harmful to the mouth and lungs, while some types of marijuana also produce toxic smoke. That toxicity can lead to cancerous changes in the mouth, tongue, throat, or lungs. And the website run by the Wales Drug and Alcohol Hotline suggests that other health conditions like bronchitis and emphysema can also come from smoking drugs.
“I have not seen any studies on this topic, but it stands to reason that any time foreign substances are breathed into the lungs, there is a risk for damage to the respiratory system,” Hoover says. “Does it cause cancer or COPD at the same rate as smoking tobacco? I’m not sure how much this has been studied.”
Taking in drugs through nasal passages (i.e., “snorting”) puts intoxicating substances into the bloodstream almost immediately. But the tissues inside the nose and throat can take the brunt of each hit, and sometimes, they can collapse and/or die off due to constant use of drugs. People who use cocaine through their noses may, for example, experience a collapse of the cartilaginous structure that holds the nose in place, as those tissues may be starved for blood and nutrition due to the constant presence of drugs.
Similar to the way people who inject drugs share needles to inject drugs, people who snort drugs may share their sniffing tools. According to the Trip Project in Canada, sharing tools can lead to cross-contamination of blood products, and that could lead to the spread of diseases like hepatitis and HIV. Every time a person shares tools, this risk can go up. Without proper treatment, some of these diseases can be life-threatening.
What’s the difference between a side effect and a withdrawal symptom?
Side effects and withdrawal symptoms tend to be very different. Side effects tend to appear during the time people take a drug, whereas withdrawal symptoms take hold after a period of time following the last dose of a drug, when the body in transitioning to sobriety. For example, an article in Pain Physician suggests that side effects linked to opioids include dizziness, slow breathing, and constipation. Withdrawal symptoms associated with opioids, on the other hand, are often compared to flu symptoms. People feel nauseated, weak, and sweaty.

How does having a chronic disease contribute to the effects and dangers of drug use?
Living with a persisting or recurring disease often means attending to a number of medical details, including:
- Doctor and lab appointments;
- Dietary restrictions;
- Prescription drug use; and
- Exercise routines.
People who attend to their condition with care and diligence might keep their health concern under control, but an addiction
can inject an element of chaos into life. People might slip on managing their health details, and that could allow the
medical condition to grow much more severe in a short period of time.
What are the health concerns of mixing drugs and alcohol?
The National Institute on Alcohol Abuse and Alcoholism reports that mixing alcohol with medications can cause all sorts of side effects, including nausea, headaches, drowsiness, and loss of coordination. In extreme cases, mixing medications with alcohol can boost the risk of internal bleeding, breathing difficulties, and heart problems. Mixing alcohol with illicit drugs is no less risky, as some drugs are strengthened by alcohol. Opioids, for example, are already sedating. Adding the sedation of alcohol to this already sedating drug can lead to issues like coma.
What are needle exchange programs, and why do they exist?
Many of the health risks involved with injecting drugs concern infection. Specifically, people who use needles to take drugs may share their needles with other drug users. Sometimes, those shared needles contain specs of blood borne pathogens, including those associated with hepatitis or AIDS. Needle exchange programs allow people who inject drugs to gain access to clean, safe needles. These programs aren’t designed with the primary objective of promoting abstinence, but people who use these programs may be encouraged to enroll in treatment each time they come in for new needles.
Are there over-the-counter medications to treat a drug overdose?
It is legal to purchase the opioid overdose reversal medication naloxone (Narcan) without a prescription in most states, however it’s only available at a pharmacy and a pharmacist must give medication administration instructions.

Can excessive drug use cause irreversible damage to the body?
In some cases, yes. People who consume large quantities of alcohol over a very long period of time, for example, can develop severe liver disease and hepatic cancer. According to the U.S. National Library of Medicine, some people need liver transplants, as their livers cannot be treated. But many of the medical concerns caused by drug use can be either controlled or eradicated with the right treatment plan. Fears about irreversible health problems shouldn’t keep people out of treatment. Proper care can always improve the situation.
Can drug use cause permanent brain damage?
Some drugs can cause damage to cells inside the brain. The National Institute on Drug Abuse says these drugs have all been associated with neurological damage:
- ayahuasca
- cocaine
- DMT
- DXM
- GHB
- heroin
- inhalants
- ketamine
- khat
- kratom
- LSD
- marijuana
- MDMA
- mescaline (peyote)
- methamphetamine
- PCP
- prescription opioids
- prescription sedatives
- prescription stimulants
- psilocybin
- Rohypnol
- salvia
- steroids (appearance- and performance-enhancing drugs)
- synthetic cannabinoids
- synthetic cathinones
- tobacco/nicotine
Unfortunately, some of the damage caused by these drugs can be permanent. Any substance with respiratory depressing effects could lead to a dose-dependent increased risk of respiratory arrest and starve the brain of enough oxygen that it could lead to brain injury and permanent brain damage.
Other brain cell issues, however, can be treated with medications and diet changes. Much of that depends on the amount of time the brain cells have been exposed to drugs, along with the type of drugs people have taken.
Conclusion
“I would like addicted people to know that they have a right to a substance-free quality of life, there is hope for them
to achieve their dreams, and they are worth the effort it takes to live in recovery,” Hoover says.
That is a message that’s easy to forget. Substances of abuse can seem so powerful and so overwhelming that people might find it difficult to fight back, despite the health consequences the use can cause. But many of the medical concerns here can be treated, and addiction can be effectively managed. People can, and should, fight back. Their physical and mental health depends upon it.
- Central Nervous System
- Chemical Imbalance
- Dental Health Due to Drug Use
- Drugs and Cholesterol
- Effects of Use to the Nose
- What Drugs Can Do to the Skin
- Drug Induced Coma
- Permanent Effects of Abuse
- Reversing Alcohol Damage
- Signs of Use in the Eyes
- Effects on the Skeletal System
- Concerns of Heart Disease
- HIV and Aids from Drug Use
